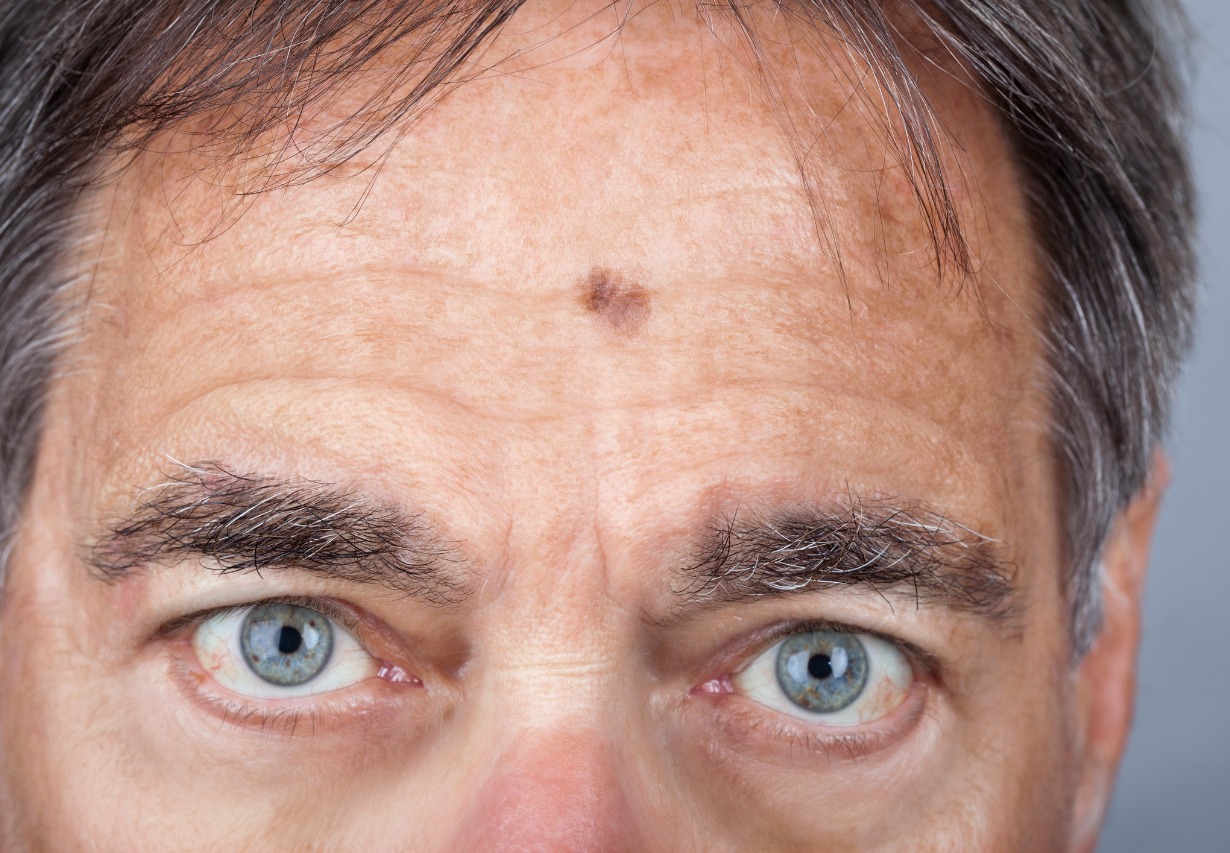
Lentigo Maligna
Lentigo maligna is a precancerous skin condition and a precursor to lentigo maligna melanoma, an invasive and serious type of skin cancer. Exposure of the skin to the sun is the primary risk factor for developing lentigo maligna. Lentigo maligna is typically slow-growing and is usually harmless, but lentigo maligna melanoma can become aggressive and spread rapidly. Recognizing the symptoms of this skin condition is critical for seeking treatment early on. Contact our dermatologists in Gainesville with Gainesville Dermatology & Skin Surgery to schedule an appointment and to learn more about our available treatments for an encompassing range of skin conditions.
Contact our Gainesville dermatology practice today to schedule a dermatology appointment and to learn more about treatment for lentigo maligna, lentigo maligna melanoma, and other skin conditions.
What Is Lentigo Maligna?
Lentigo maligna, sometimes called Hutchinson's melanotic freckle, is a precancerous skin condition and a precursor to lentigo maligna melanoma, a dangerous form of skin cancer. In this early form of skin cancer, the malignant cells are confined to the epidermis, the skin's outer surface. When it starts growing under the skin's surface, it develops into maligna melanoma, the least common type of melanoma. Lentigo maligna occurs in sun-damaged skin and is generally found on the neck and face, especially on the nose and cheeks.
This precancerous skin condition is usually harmless and slow-growing, often expanding in diameter over 5–20 years. Lentigo maligna melanoma, however, can spread aggressively. It is important to recognize the symptoms of these conditions for treatment as early as possible.
Who Gets Lentigo Maligna?
The risk of lentigo maligna relates closely with sun damage to skin. As such, lentigo maligna is more common in those who spend a significant amount of time outdoors, those who work outdoors, older individuals, and those associated with solar damage and basal cell carcinoma and squamous cell carcinoma (keratinocyte skin cancer). Although lentigo maligna often occurs in people with very fair skin, it can also occur in those with any skin type and tone variation.
It is rare, however, in those with brown and black skin. Lentigo maligna is typically more common in males than in females. Most patients diagnosed with lentigo maligna are older than 40 years of age, with the peak age of diagnosis ranging from 60–80 years of age. Unlike other forms of melanoma and precancerous skin conditions, lentigo maligna is not related to a person's number of moles or atypical moles.
What Does Lentigo Maligna Look Like?
The visual symptoms of lentigo maligna are similar to those of lentigo maligna melanoma. These conditions appear as a flat or somewhat raised brown patch on the skin, similar to a freckle or an age spot. These lesions have a smooth surface with an irregular shape or border. They are usually a shade of brown, though they may also be pink, red, or white. Compared with other types of skin cancer, lentigo maligna and lentigo maligna melanoma produce large-sized lesions. The lesions are usually a minimum of 6 millimeters wide and can grow to encompass several centimeters of skin.
It most commonly presents on the face or neck, especially the nose and cheeks, though it can appear elsewhere on the body. Due to its appearance, it can be difficult to distinguish lentigo maligna and lentigo maligna melanoma from freckles or age spots just by looking at the lesion. It can also be difficult to visually differentiate between lentigo maligna and lentigo maligna melanoma. Lentigo maligna melanoma usually features increased thickness, multiple colors (black and blue), bleeding, itching, and stinging.